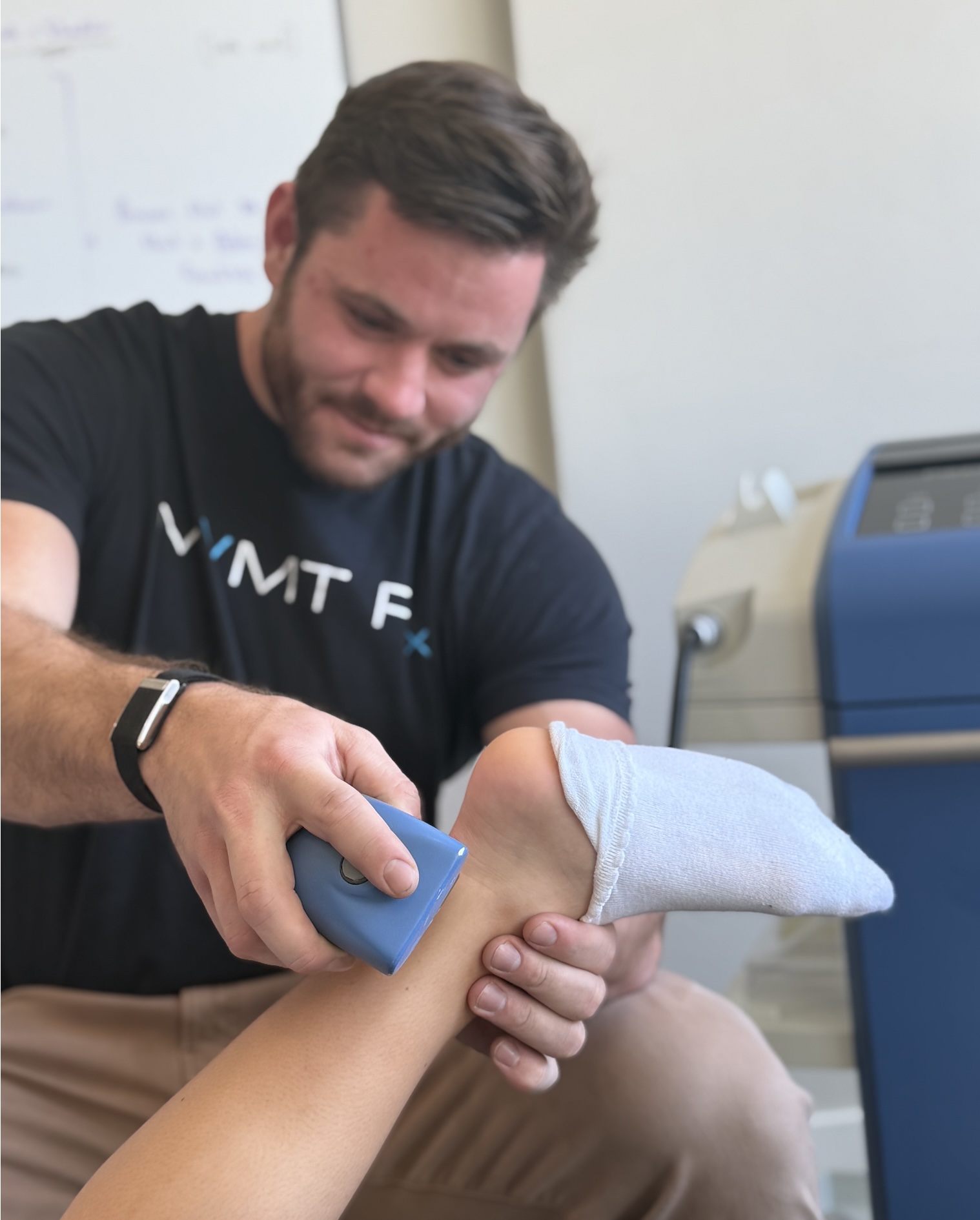
Shockwave Therapy & Achilles Tendinitis
Achilles Tendinitis: Why Rest and Stretching Are Making It Worse
You have been resting. Stretching your calves. Wearing the heel lifts. Maybe you even got an injection. And your Achilles still hurts every time you push off, go upstairs, or try to get back to running. Here is why — and what actually works.
The Pattern
The Rest Trap That Keeps Your Achilles Stuck
It started gradually. A stiffness in the back of your ankle first thing in the morning. A tightness after sitting for a while that loosened up once you walked around. You ignored it — because that is what active people do. Then it got worse. Now it hurts during walks. It hurts going up stairs. It hurts pushing off to jog. And the thing that used to warm up and feel better is now present all the time.
So you went to your doctor. Or your PT. Or your chiropractor. And you were told to rest, stretch your calves, maybe wear a heel lift, take anti-inflammatories, and wait. You did all of it. Weeks went by. Months went by. The stiffness might have improved slightly, but the moment you tried to do anything meaningful — a hike, a run, a pickup game, even yard work — it flared right back up. Exactly where it was. As if all that rest accomplished nothing.
Because it did accomplish nothing.
Rest does not fix Achilles tendinopathy. It removes the symptom temporarily by removing the load — but it does nothing to address the structural changes in the tendon that are causing the problem. When you rest a degenerative tendon, you are not healing it. You are deconditioning it further. You are making the tendon weaker, less tolerant, and more vulnerable to the next time you try to load it. And the cycle starts again.
If you are in Reno or Sparks and you have been dealing with Achilles pain for more than a few months, you are almost certainly past the point where rest, stretching, and anti-inflammatories can help. What you are dealing with is a tendon that has structurally changed — and the only way to change it back is to load it correctly.
Common experiences patients describe before finding MVMT Rx: morning stiffness in the Achilles that takes several minutes to loosen up, pain at the back of the heel or just above it that gets worse with stairs and inclines, failed calf stretching programs that never made a lasting difference, cortisone injections that were either refused by their doctor or provided only temporary relief, being told to stop running or stop hiking without any plan to get back, months of rest that made the tendon feel weaker not stronger, and the growing fear that their active lifestyle is slipping away.
What the Evidence Says
What the Research Actually Says About Achilles Tendinitis
The first thing to understand is that the word "tendinitis" is misleading. The suffix "-itis" implies inflammation — and in the early stages of an Achilles injury, inflammation may play a role. But by the time most patients are three or more months in, inflammation is no longer the primary driver. What is happening in the tendon is degeneration: disorganized collagen fibers, areas of cell death, neovascularization (the growth of new, poorly formed blood vessels that actually increase pain sensitivity), and a loss of the tendon's normal mechanical properties. The more accurate clinical term is tendinopathy — a structural disease of the tendon, not a simple inflammation problem.[1]
This distinction matters because treatments designed for inflammation — rest, ice, anti-inflammatories, cortisone — do not address degeneration. They suppress symptoms while the structural problem persists underneath. A 2007 Cochrane review found that nonsteroidal anti-inflammatory drugs (NSAIDs) provide no meaningful benefit for chronic Achilles tendinopathy beyond short-term pain relief, and no evidence supports their use in promoting tendon healing.[2]
Cortisone injections deserve a direct conversation. Many providers avoid injecting the Achilles entirely — and for good reason. A 2010 systematic review found that corticosteroid injections around the Achilles tendon carry a significant risk of tendon rupture, particularly in patients with pre-existing tendinopathy.[3] The Achilles is the largest and most heavily loaded tendon in the body. Injecting a degenerative tendon with a substance that further weakens collagen structure is not conservative care — it is a gamble with catastrophic downside. If your Achilles ruptures, you are looking at months of immobilization, possible surgical repair, and a recovery timeline that dwarfs whatever the tendinopathy would have required. And yet patients are still offered cortisone for chronic Achilles pain without being clearly told the risk.
The second thing to understand: the gold standard for Achilles tendinopathy treatment — based on decades of research — is progressive loading. Eccentric exercise protocols, first published by Alfredson in 1998, demonstrated that heavy, slow, eccentric calf loading could produce significant improvement in chronic Achilles tendinopathy where other treatments had failed.[4] Since then, the evidence has expanded to include heavy slow resistance training, isometric loading for pain modulation, and combined protocols that progress from pain management through full return to sport. The common thread across all of these is load — not rest.
The third piece: focused shockwave therapy. A 2015 systematic review in the American Journal of Sports Medicine found that extracorporeal shockwave therapy produces significant improvements in pain and function for chronic lower limb tendinopathies, including Achilles tendinopathy, particularly in patients who have failed conservative treatment.[5] Shockwave works by stimulating neovascularization (functional blood vessel formation, unlike the disordered neovascularization seen in diseased tendons), promoting collagen remodeling, disrupting pain signaling at the nerve level, and mechanically stimulating the tendon's healing response. At MVMT Rx, we use the PiezoWave 2 — a focused shockwave device that delivers energy precisely to the affected area of the tendon, not scattered across the surface like radial pressure wave devices that many clinics use and call "shockwave."
When shockwave therapy is combined with progressive loading — not used as a standalone passive treatment — the evidence supports significantly better outcomes than either approach alone. The shockwave addresses the tissue pathology. The loading builds the capacity the tendon needs to handle real-world demands. One without the other is an incomplete answer.
But there is a practical advantage to shockwave that most patients do not hear about: it accelerates the timeline. By stimulating tendon regeneration and reducing pain at the tissue level, shockwave therapy allows us to load the tendon more aggressively, earlier. That means progressing from the Relief and Adaptation phases into Integration — where you are actually returning to running, hiking, and sport — significantly faster than with loading alone. Without shockwave, you are waiting longer for the tendon to tolerate the demands of real-world activity. With it, we can compress that timeline because the tissue is responding faster, pain is dropping sooner, and the tendon can handle progressive challenge at a pace that matches your goals instead of holding you back.
Why the standard approach fails for chronic Achilles tendinopathy: rest deconditions the tendon instead of healing it, stretching applies tensile load without progressive dosing and can further irritate a reactive tendon, anti-inflammatories suppress symptoms without addressing structural degeneration, cortisone injections carry measurable rupture risk in weight-bearing tendons, heel lifts reduce load temporarily but create dependency without building tolerance, and most programs never progress beyond early-stage exercises — leaving patients in a permanent state of underloading.
Looking Deeper
Your Achilles Is Where the Problem Ended Up — Not Where It Started
The Achilles tendon does not work in isolation. It is the terminal structure of the entire posterior chain — everything from your lower back through your glutes, hamstrings, and calves feeds into how the Achilles loads and unloads during movement. When there are capacity deficits or motor control problems anywhere in that chain, the Achilles absorbs forces it was never designed to handle alone.
The most common upstream driver we see is calf and soleus weakness. Not tightness — weakness. The soleus in particular is the workhorse of walking, stair climbing, and any sustained lower-leg loading. Most patients with chronic Achilles tendinopathy have significant deficits in calf endurance and strength compared to their uninvolved side and compared to normative values. Nobody tested it. Nobody measured it. They were just told to stretch.
The second driver is hip and lumbopelvic control. When the hip cannot stabilize properly during single-leg stance — which is what walking and running essentially are — the lower leg compensates. The ankle pronates excessively, the Achilles takes on rotational forces it is not built for, and the medial or insertional portion of the tendon becomes overloaded. Through our training in Dynamic Neuromuscular Stabilization (DNS), we assess how well the hip centrates in the socket, how the trunk stabilizes through intra-abdominal pressure regulation, and how the pelvis and ribcage coordinate during gait. If the system above the ankle is not doing its job, no amount of calf raises will solve the problem below it.
The third driver — and one that is almost never assessed — is neural involvement. The sural nerve runs directly alongside the Achilles tendon. When this nerve becomes sensitized, restricted in its ability to slide through surrounding tissue, or irritated by local swelling and adhesion, it can amplify or even mimic Achilles tendon pain. Through clinical neurodynamics — the assessment of how nerves move, tension, and slide through the body — we can identify whether sural nerve involvement is contributing to your symptoms. If it is, the treatment approach must address the nerve, not just the tendon. Without this assessment, a significant driver of persistent Achilles pain goes unidentified.
The fourth consideration — and one that almost no provider assesses when treating Achilles tendinopathy — is midfoot mobility and foot mechanics. Your foot is not one rigid block. It is a complex system of joints that must move segmentally to absorb and distribute force. When the midfoot joints — the talonavicular, cuboid, cuneiforms — are stiff and cannot pronate through their normal range, the entire foot compensates by pronating excessively through the rearfoot. The heel rolls inward, the subtalar joint everts beyond its intended range, and the Achilles tendon — which attaches directly to the calcaneus — gets loaded asymmetrically. Instead of pulling in a clean, vertical line, it is now absorbing rotational and medial forces it was never designed to handle. Over time, this creates the overload pattern that drives insertional tendinopathy specifically.
A 2011 systematic review in the Journal of Foot and Ankle Research confirmed that individuals with Achilles tendinopathy display increased rearfoot eversion during gait — the exact compensatory pattern you would expect when midfoot segmental mobility is restricted.[6] And the clinical evidence supports direct intervention: a 2017 case report in the International Journal of Sports Physical Therapy documented a 51-year-old runner with persistent insertional Achilles tendinopathy who had failed prior PT. Treatment centered on joint mobilization targeting restricted foot and ankle joints — and the patient achieved full symptom resolution and returned to marathon running, with results maintained at one-year follow-up.[7]
This is why we adjust feet and ankles as part of our Achilles treatment plans. Restoring segmental midfoot mobility changes how force distributes through the foot during every single step. It reduces the compensatory rearfoot pronation that overloads the tendon insertion. And it allows the first ray — your big toe — to extend properly during push-off, which is critical for activating the windlass mechanism and engaging the calf and soleus through their full working range. Without midfoot mobility, your calf raises are loading a foot that cannot distribute that force correctly — and you are training compensation, not correction.
Restrictions in ankle dorsiflexion compound the problem further. When the ankle cannot bend upward adequately, the Achilles works through a compressed range of motion during every step. The tendon absorbs more strain per degree of movement. And the body compensates by pronating harder through the rearfoot — reinforcing the exact overload pattern that caused the problem. These are not issues that orthotics solve. They are mobility and motor control deficits that need to be assessed, measured, and restored directly.
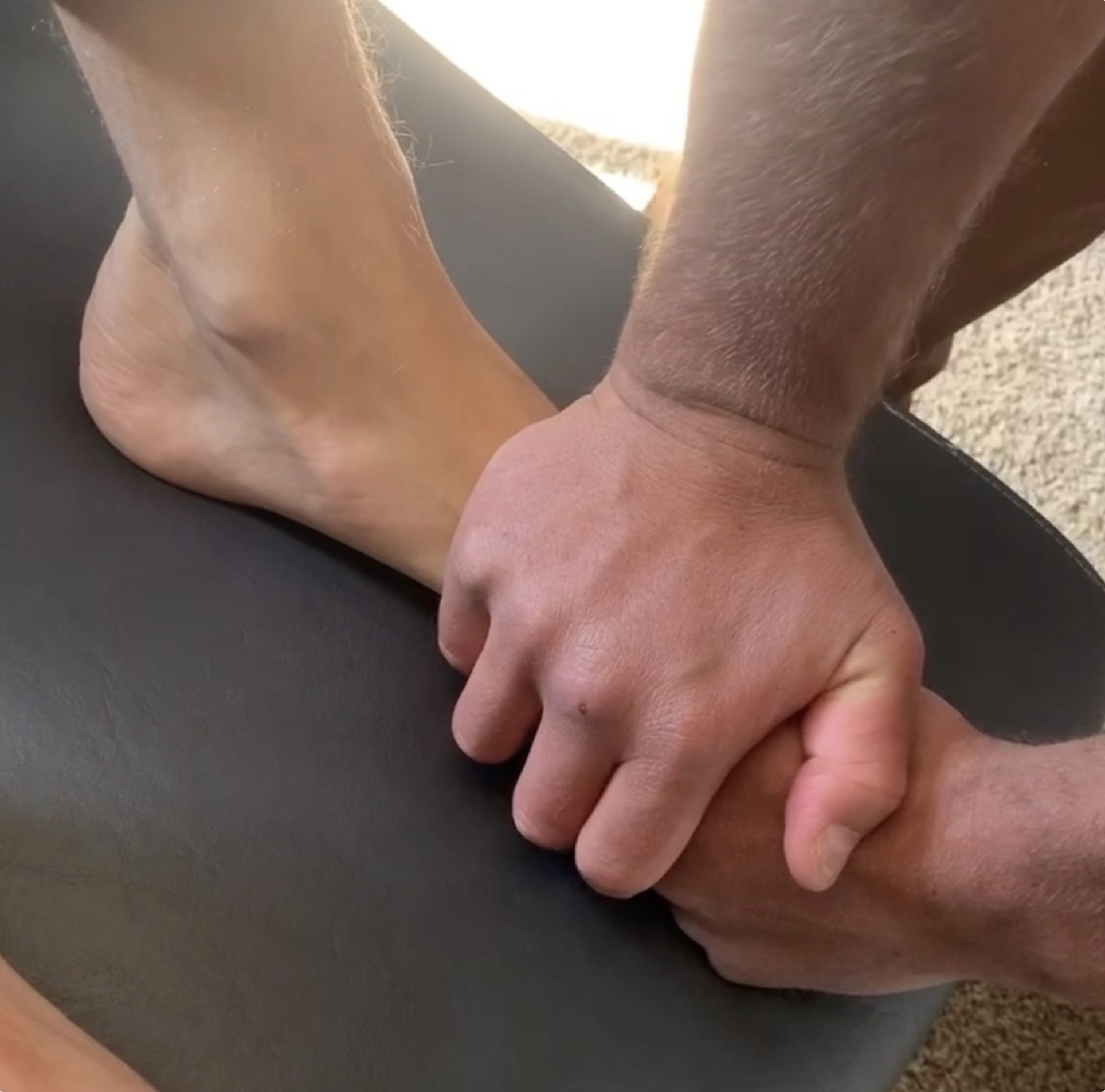
Restoring midfoot segmental mobility — reducing compensatory rearfoot pronation that overloads the Achilles insertion.

When midfoot joints lose mobility, the rearfoot compensates — overloading the Achilles insertion.
Root causes we commonly find driving chronic Achilles tendinopathy: calf and soleus strength deficits that were never tested or addressed, hip instability and lumbopelvic control deficits that overload the lower leg during gait, sural nerve sensitization or restriction mimicking or amplifying tendon pain, midfoot joint stiffness causing compensatory rearfoot pronation and asymmetric Achilles loading, restricted first ray extension disrupting the windlass mechanism and calf activation, ankle dorsiflexion limitations that compress the Achilles working range, poor single-leg balance and proprioception that increase tendon strain with every step, and deconditioning from months of rest that leaves the tendon weaker than before treatment started.
We use objective measurements — dynamometer testing for calf and soleus strength, ankle dorsiflexion range of motion, manual palpation of every individual bone and joint in the foot and ankle to identify restrictions, limb symmetry comparison, and functional movement analysis under load — to quantify exactly where the deficits are. When we find joints that are not moving properly, we adjust them directly to restore segmental mobility. We calculate side-to-side symmetry and compare your results to normative data derived from hundreds of thousands of pain-free active adults, using torque values that account for your body weight and limb length. That data drives the plan. Not a protocol. Not a guess. Not an MRI.
A Different Approach
How We Actually Fix Achilles Tendinitis That Nothing Else Has Fixed
At MVMT Rx, we use a clinical reasoning framework called the RAIL System that guides every decision we make — from your first visit through long-term resolution. For Achilles tendinopathy, this framework is what separates a care plan that keeps you resting indefinitely from one that actually rebuilds the tendon and gets you back to the activities that matter.
Relief — The first priority is calming the tendon down enough to start loading it. This is where focused shockwave therapy with the PiezoWave 2 plays a critical role — stimulating the tendon's healing response, promoting functional neovascularization, disrupting pain signaling, and beginning the process of collagen remodeling. We may also use Class IV laser therapy to reduce local pain and support tissue recovery, isometric loading for immediate pain modulation (isometric calf holds have been shown to produce significant acute pain reduction in tendinopathy), and targeted soft tissue work to address sural nerve restrictions or calf adhesions. We restore midfoot and ankle joint mobility through chiropractic adjustments — correcting the mechanical environment the tendon operates in. Relief matters — but it is the starting line, not the finish.
Adaptation — Once the tendon is tolerating basic load, we begin building capacity. This is where the real work starts. Heavy slow resistance training for the calf complex — specifically the gastrocnemius and soleus — using progressive dosing based on your objective testing. We measure calf strength with dynamometry, compare side-to-side, track progress session to session, and dose your loading based on data, not guesswork. We simultaneously address the upstream drivers: hip stability through DNS-based training, lumbopelvic control, single-leg balance, ankle mobility, midfoot joint restrictions, and any neural involvement identified through our neurodynamic assessment. This phase is about rebuilding the tissue's tolerance to load — systematically and measurably.

Progressive calf loading on wedges — building the tendon capacity that rest and stretching never will.
Integration — This is where you earn the right to do the things that matter to you. Running. Hiking. Playing pickleball. Going up and down trails without thinking about your Achilles. We introduce plyometric loading, sport-specific movement patterns, reactive agility, and progressive return-to-run protocols — all guided by objective testing that tells us whether your tendon is ready for each new demand. We do not guess when you are ready to return to activity. We measure it.
Lifespan — You graduate with a tendon that is stronger than it was before the injury and a body that knows how to maintain it. You understand what loading your Achilles needs to stay healthy, what your calf complex requires to protect it, and how to manage flare-ups if they occur — without panicking and without running back to a provider every time something feels off. This is physical freedom. This is the skillset that keeps you hiking, running, traveling, and staying active for decades — whether you are pushing through a trail in Tahoe, keeping up with your family on vacation, or simply trusting your body to handle whatever life throws at you.
Shockwave and rest are Phase 1 — not the entire plan.
What This Looks Like
What an Achilles Tendinitis Plan Actually Looks Like at MVMT Rx
Every patient is different, but here is the general shape of how we approach persistent Achilles tendinitis — the kind that has not responded to rest, stretching, heel lifts, or the "just wait it out" advice you have been following for too long.
Step 1 — Free Discovery Call: A phone call where we learn about your situation — how long you have been dealing with Achilles pain, what you have tried, what has failed, and what activities you are missing. We answer your questions, explain how our approach is different, and determine whether it makes sense to meet in person. No commitment. No pressure. Just a real conversation to see if we are the right fit.
Step 2 — Free Discovery Visit: A 60-minute, in-person assessment where we walk through your full history — including every provider you have seen, every treatment you have tried, and every activity you have modified or given up because of your Achilles. We perform a functional evaluation of the entire lower extremity chain — not just the tendon — and give you a clear picture of what is actually driving your pain. We assess calf and soleus strength, ankle dorsiflexion, midfoot segmental mobility, hip stability, single-leg balance, nerve mobility, and how your body distributes force during gait. This is a root cause assessment, not a sales pitch. The goal is mutual confidence that you are in the right place and we can help.
Step 3 — Evaluation and First Treatment: If we both agree it is the right fit, we complete the clinical picture with additional assessment, then turn everything into a structured treatment session so you can experience firsthand what a high-intention, 60-minute session looks like — shockwave therapy, chiropractic adjustments to the foot and ankle, targeted loading, and clinical coaching in the same visit. From there, we make a clinical recommendation on a plan of care — including time, frequency, and investment — decided together.
Ongoing Care: Every session is 60 minutes, one-on-one with your doctor. Your plan adapts weekly based on how your tendon responds. Shockwave therapy is used strategically during the Relief phase — not as a standalone fix — and paired with progressive rehabilitation that builds real capacity between visits. You receive programming to follow at home, at the gym, or on the road. You are coached, progressed, and held accountable through every phase of recovery. And you develop the movement literacy and body awareness to confidently manage your own Achilles for life — not depend on someone else to keep it feeling decent.
What an Achilles tendinopathy plan at MVMT Rx may include: focused shockwave therapy with the PiezoWave 2, chiropractic adjustments to midfoot and ankle joints, Class IV laser therapy for tissue-level pain reduction, isometric calf loading for acute pain modulation, heavy slow resistance training for calf and soleus capacity, sural nerve mobilization through clinical neurodynamics, DNS-based hip centration and lumbopelvic control training, ankle dorsiflexion and first ray mobility restoration, progressive return-to-run and plyometric loading protocols, dynamometry-based objective retesting to track measurable progress, and ongoing plan adaptation based on your response.
Learn More: Focused Shockwave Therapy at MVMT Rx →
How we use PiezoWave 2 focused shockwave therapy — not radial pressure wave — as part of the RAIL System for tendinopathy in Reno and Sparks, NV.
Read the Full Guide: Why a Multi-Modal Approach Works →
Our complete breakdown of the RAIL System, our clinical toolkit, and why single-modality care fails for chronic pain.
Related: Why Your Plantar Fasciitis Won't Go Away (And What Actually Works) →
Focused shockwave therapy, progressive loading, and clinical neurodynamics — why the stretch-ice-rest cycle fails for chronic heel pain.
Related: Why Your Low Back Pain Keeps Coming Back After Every Adjustment →
The same adjustment-plus-rehab approach applied to chronic low back pain — DNS, McKenzie, and progressive loading.
Related: Knee Osteoarthritis — Why Generic Exercise Programs Fail →
Why your X-ray does not define your ceiling, and how objective testing and progressive loading change the outcome for knee OA.
Related: Why Your Shoulder Isn't Getting Better →
Rotator cuff tears, impingement, and frozen shoulder — why passive care fails and what objective-driven rehabilitation actually looks like.
Related: Neck Pain After Failed Chiropractic Care →
Why adjustments alone do not resolve chronic neck pain, and how McKenzie assessment, clinical neurodynamics, and progressive rehabilitation change the outcome.
Related: Hip Pain — Why Stretching and Foam Rolling Aren't Fixing Your Hips →
Clinical myofascial release, DNS, and progressive hip rehabilitation — why self-stretching fails for chronic hip pain.
Related: Herniated Disc — What Your MRI Isn't Telling You →
Class IV laser therapy, McKenzie assessment, neurodynamics, and progressive loading — why rest and fear make disc herniations worse.
Related: The Hidden Cost of Daily Tylenol and NSAIDs →
What the research says about daily OTC painkiller use — liver damage, GI bleeding, cardiovascular risk, delayed healing, and why your pain deserves a better answer than medication.
Frequently Asked Questions
Achilles Tendinitis Questions We Hear Every Week
How long does Achilles tendinitis take to heal?
Chronic Achilles tendinitis typically requires 3 to 6 months of structured progressive loading to achieve meaningful, lasting improvement. The timeline depends on how long you have had the condition, how much deconditioning has occurred, and whether upstream drivers like hip stability and calf strength are addressed. The key difference in our approach is that you are actively improving throughout — not passively waiting for healing that never comes.
Is shockwave therapy painful?
Focused shockwave therapy produces a deep, pulsing sensation at the treatment site. Most patients describe it as intense but tolerable — a 4 to 6 out of 10 during treatment. The discomfort typically subsides immediately after the session. At MVMT Rx, we use the PiezoWave 2, which delivers focused energy precisely to the affected tissue rather than scattering it across the surface like radial pressure wave devices. This means more effective treatment with less collateral discomfort.
Should I get a cortisone injection for my Achilles?
This is a conversation to have with your provider, but the evidence is clear: cortisone injections around the Achilles tendon carry a measurable risk of tendon rupture, particularly in tendons that are already degenerative. Many orthopedic surgeons and sports medicine physicians avoid Achilles cortisone injections entirely for this reason. If you have been offered one, ask your provider directly about the rupture risk and whether progressive loading and shockwave therapy have been considered as alternatives.
Can I still exercise with Achilles tendinitis?
Yes — and in most cases, you should. Complete rest is one of the least effective strategies for chronic tendinopathy because it further deconditions the tendon. The key is modifying your activity to stay within the tendon's current tolerance while progressively building that tolerance over time. We help you identify what activities you can continue, what to modify, and how to load the tendon in a way that promotes healing rather than aggravating it.
My doctor told me I have a partial Achilles tear. Does that mean I need surgery?
Not necessarily. Many partial tears — particularly small, chronic ones — respond well to structured progressive loading and shockwave therapy. The presence of a partial tear on imaging does not automatically dictate a surgical outcome. The decision should be based on the size and location of the tear, your functional capacity, your response to conservative care, and your specific goals. Our evaluation helps you understand exactly where you stand and what options make the most sense for your situation.
What is the difference between insertional and midportion Achilles tendinitis?
Insertional tendinopathy affects the point where the Achilles attaches to the heel bone (calcaneus) and is often associated with calcification, Haglund's deformity, or retrocalcaneal bursitis. Midportion tendinopathy affects the body of the tendon, typically 2 to 6 centimeters above the insertion. Both respond to progressive loading, but the specific loading protocols, the role of shockwave therapy, and the management of compressive forces differ between the two. Our evaluation identifies which type you have and tailors the approach accordingly.
I have had Achilles pain for over a year. Is it too late?
No. We routinely work with patients who have had Achilles tendinopathy for one, two, or even three or more years. Chronic does not mean permanent. The tendon retains the ability to remodel and adapt to load regardless of how long the condition has been present. It may take longer to reach full capacity, but the process works — because you are addressing the tissue pathology directly instead of waiting for it to resolve on its own.
What is different about MVMT Rx compared to the PT or chiropractor I have already seen?
Three things. First, every session is 60 minutes, one-on-one with your doctor — you are never handed off to an aide or technician. Second, we combine focused shockwave therapy, chiropractic adjustments, progressive rehabilitation, clinical neurodynamics, DNS, laser, and foot and ankle mobilization under one roof — in the same session. Third, we use objective testing — dynamometry, range of motion, side-to-side comparison — and a clinical reasoning model called the RAIL System to guide every decision — not generic protocols, not arbitrary visit counts, and not insurance authorization timelines.
Conditions and symptoms we treat at MVMT Rx related to Achilles tendinopathy: chronic Achilles tendon pain, Achilles tendinitis, Achilles tendinosis, insertional Achilles tendinopathy, midportion Achilles tendinopathy, Achilles tendinopathy treatment and rehabilitation in Reno and Sparks NV, focused shockwave therapy for Achilles tendinopathy (PiezoWave 2 / EPAT), failed conservative treatment for Achilles pain — rest stretching and cortisone, cortisone injection risk for Achilles tendon — rupture weakening and degeneration, eccentric calf loading and heavy slow resistance for Achilles rehab, partial Achilles tear conservative treatment vs surgery, calf and soleus strengthening for Achilles rehabilitation, hip stability lumbopelvic control and DNS for lower extremity tendinopathy, sural nerve involvement mimicking or amplifying Achilles tendon pain, clinical neurodynamics for persistent Achilles and ankle pain, ankle dorsiflexion limitation and Achilles overload, midfoot joint mobilization and foot adjustment for Achilles tendinopathy, compensatory rearfoot pronation and Achilles overload, first ray extension windlass mechanism and calf activation, Haglund's deformity retrocalcaneal bursitis and calcific Achilles tendinopathy, return to running after Achilles tendinopathy — progressive loading protocols, foot and ankle chiropractic adjustment for tendon pain Reno NV, MVMT Rx Sports Care and Chiropractic — Achilles tendinopathy specialist Reno NV, and sports chiropractor and performance rehab for active adults in Reno and Sparks.
References
- Maffulli N, Khan KM, Puddu G. Overuse tendon conditions: time to change a confusing terminology. Arthroscopy. 1998;14(8):840–843. doi:10.1016/S0749-8063(98)70021-0
- McLauchlan GJ, Handoll HH. Interventions for treating acute and chronic Achilles tendinitis. Cochrane Database of Systematic Reviews. 2001;(2):CD000232. Updated 2007. doi:10.1002/14651858.CD000232
- Coombes BK, Bisset L, Vicenzino B. Efficacy and safety of corticosteroid injections and other injections for management of tendinopathy: a systematic review of randomised controlled trials. The Lancet. 2010;376(9754):1751–1767. doi:10.1016/S0140-6736(10)61160-9
- Alfredson H, Pietilä T, Jonsson P, Lorentzon R. Heavy-load eccentric calf muscle training for the treatment of chronic Achilles tendinosis. American Journal of Sports Medicine. 1998;26(3):360–366. doi:10.1177/03635465980260030301
- Mani-Babu S, Morrissey D, Waugh C, et al. The effectiveness of extracorporeal shock wave therapy in lower limb tendinopathy: a systematic review. American Journal of Sports Medicine. 2015;43(3):752–761. doi:10.1177/0363546514531911
- Munteanu SE, Barton CJ. Lower limb biomechanics during running in individuals with Achilles tendinopathy: a systematic review. Journal of Foot and Ankle Research. 2011;4:15. doi:10.1186/1757-1146-4-15
- Jayaseelan DJ, Post AA, Mischke JJ, Sault JD. Joint mobilization in the management of persistent insertional Achilles tendinopathy: a case report. International Journal of Sports Physical Therapy. 2017;12(1):133–143. PMID: 28217424
Done Resting a Tendon That Needs to Be Loaded?
If you have been dealing with Achilles pain for months and nothing has worked, the approach needs to change — not your effort. Start with a free conversation.
Book Your Free Discovery CallMVMT Rx Sports Care & Chiropractic | Reno & Sparks, NV | (775) 245-4142

Free Guides
Patient Care
Links
© Copyright 2026. MVMT Rx Sports Care & Chiropractic. All Rights Reserved.